Breast Imaging
Breast imaging tools contribute to the early detection and diagnoses of breast abnormalities like breast cancer.
Digital Mammography
Females at average risk should begin getting their first mammogram at age 40 and continue to do so on an annual basis. While screening mammogramsA low dose x-ray picture of the breast that allows a doctor to view glandular tissue and determine the presence of cancer. are routinely administered to detect breast cancer in those who have no apparent symptoms, diagnostic mammograms are used after suspicious results on a screening mammogram or after some signs of breast cancer alert the physician to check the tissue.

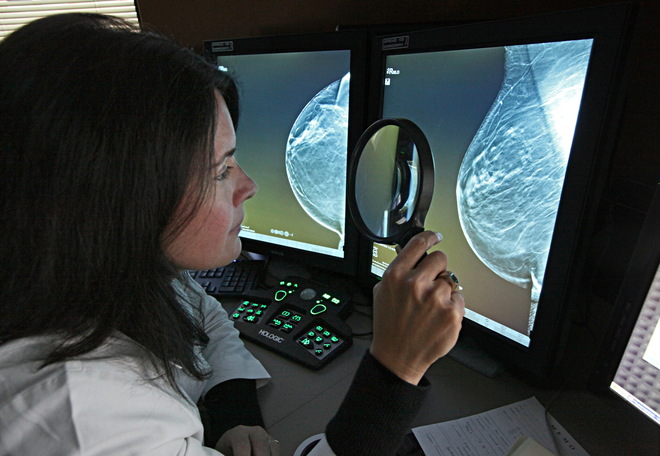
Mammogram Tips:
- When possible, schedule yourself for a breast tomosynthesis, also known as 3D mammography. This is an advanced technology that takes multiple images of breast tissue to recreate a 3-dimensional picture of the breast, resulting in additional cancers being detected while lowering false-positiveA test result that indicates that a person has a disease when the person does not have that disease. readings.
- If applicable, schedule your mammogram at the end of your menstrual cycle when your breasts are least tender. The readings will be more accurate, the compression will be more comfortable, and when they compare films from year to year, they will be comparing breasts of similar status.
- When possible, go to the same imaging center each year. If you move or change sites, bring your digital records with you, so that current mammograms can be compared to past images.
- Make sure the center that is doing your mammogram is accredited by the American College of Radiology. This will ensure that accurate and safe dosages of radiation are being used.
- High-risk individuals may benefit from starting breast cancer screening at a younger age and supplementing annual screening mammography with a yearly breast MRI.
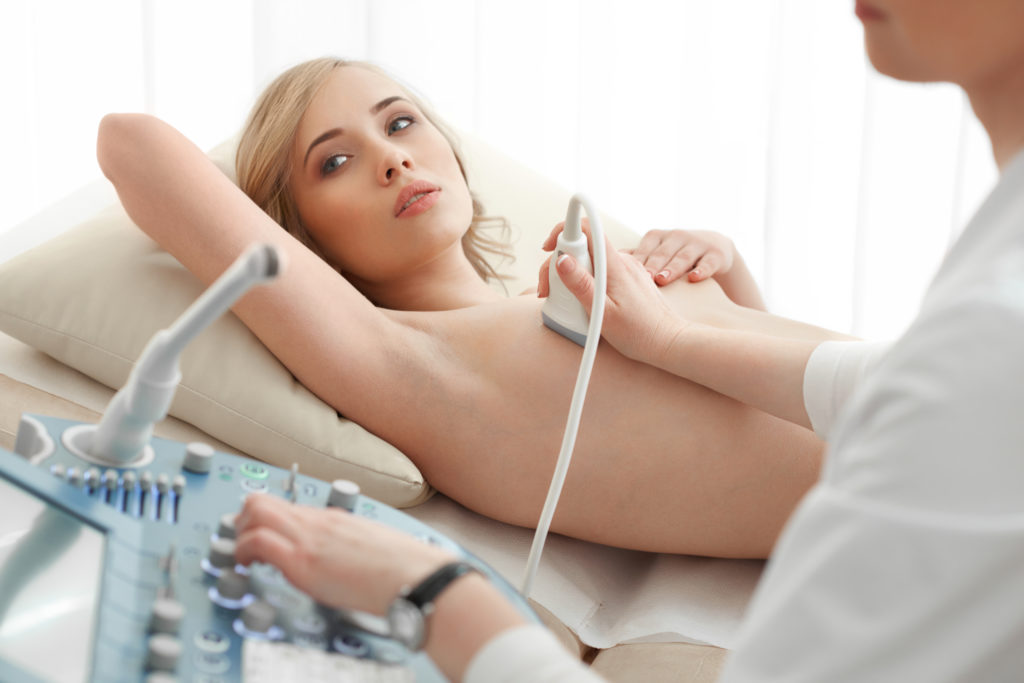
Breast Ultrasound
The sonographer or radiologist then glides a transducer, a small hand-held instrument, over the breast. The breast ultrasound uses sound waves to distinguish solid and fluid-filled masses. For example, a breast ultrasound can detect cysts which are fluid-filled, noncancerous masses.
Some physicians may require their patients to schedule a breast ultrasound with their routine mammography. The combined screening also detected more cancers with dense breast tissue, which can make it difficult to see cancers on a mammogram.
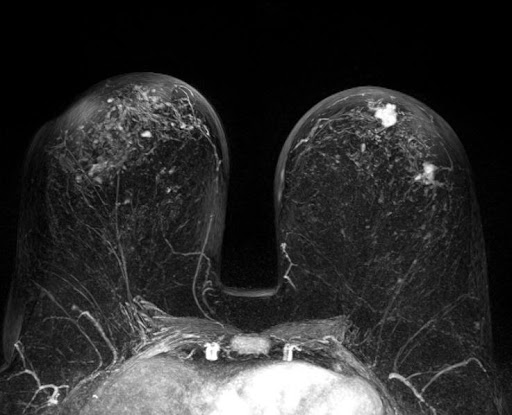
Breast MRI
A breast MRI is sometimes used for someone who already has been diagnosed with breast cancer, to help measure the size of the cancer, look for other tumors in the same breast, and to check for tumors in the opposite breast. But not everyone who has been diagnosed with breast cancer needs a breast MRI.
Although an MRI can find some cancers not seen on a mammogram, it’s also more likely to find things that turn out not to be cancer (called a false positive). This can result in a person getting tests and/or biopsies that end up not being needed. Therefore, an MRI is not recommended as a screening test for people at average risk of breast cancer.